Summer in Melbourne often means warm evenings, outdoor sport and long days at the park. For many families, it also means itchy eyes, runny noses and hayfever. Children across Melbourne and regional Victoria can have blocked noses and sneezing for weeks at a time when pollen counts are high.
During these months, parents frequently notice that their child snores at night and naturally assume it is just part of their allergies. For some children that is true. A blocked nose leads to mouth breathing, and mouth breathing can be noisy.
However, when snoring is loud, regular or carries on after allergy symptoms have settled, it may be a sign of a deeper problem. Sometimes summer snoring draws attention to underlying issues with tonsils, adenoids and sleep disordered breathing that have been present for longer than parents realise.
This article explains how allergies, enlarged tonsils and adenoids and sleep disordered breathing fit together, and when it may be helpful to organise an ENT assessment.
Why this topic matters for families in Melbourne
Sleep is one of the foundations of a child’s wellbeing. During deep sleep, the brain processes memories, hormones that support growth are released, and the body recovers from the day. If breathing is repeatedly disturbed, even for a few seconds at a time, that deep sleep can be interrupted.
Over time, poor quality sleep can affect a child’s mood, behaviour and learning. Teachers may notice that a child is more distracted or emotional. Parents might see more meltdowns, clinginess or arguments over small things. In a busy city like Melbourne, where school, sport and family schedules are already demanding, these problems can have a real impact on daily life.
Recognising when snoring is more than a temporary side effect of hayfever allows parents to seek help earlier and protect their child’s long term health.
Introducing the specialists
Melbourne ENT is a specialist ear, nose and throat clinic based in St Kilda East. The clinic cares for both adults and children with ENT and head and neck concerns, including snoring, enlarged tonsils and adenoids and sleep disordered breathing.
The practice is led by two experienced ENT surgeons.
Dr Stephen Kleid is an ENT and Head & Neck Surgeon. He graduated from the University of Melbourne and completed advanced surgical training at major centres including Royal Melbourne Hospital, the Royal Children’s Hospital, the Eye and Ear Hospital and St Vincent’s Hospital. He has many years of experience managing complex head and neck conditions as well as nasal and throat problems and continues to teach and supervise surgical trainees.
Dr Simon Braham is an ENT Surgeon who trained in Melbourne and has worked in both public and private hospitals across Victoria, including the Royal Victorian Eye and Ear Hospital and regional centres. He has a strong interest in nasal and sinus surgery and paediatric ENT, including surgery for children who snore or have enlarged tonsils and adenoids.
Together, Dr Kleid and Dr Braham provide thorough assessment and evidence based care at Melbourne ENT, working closely with GPs and paediatricians throughout Melbourne and regional Victoria.
Understanding Snoring in Children
✓ What actually causes the snoring sound
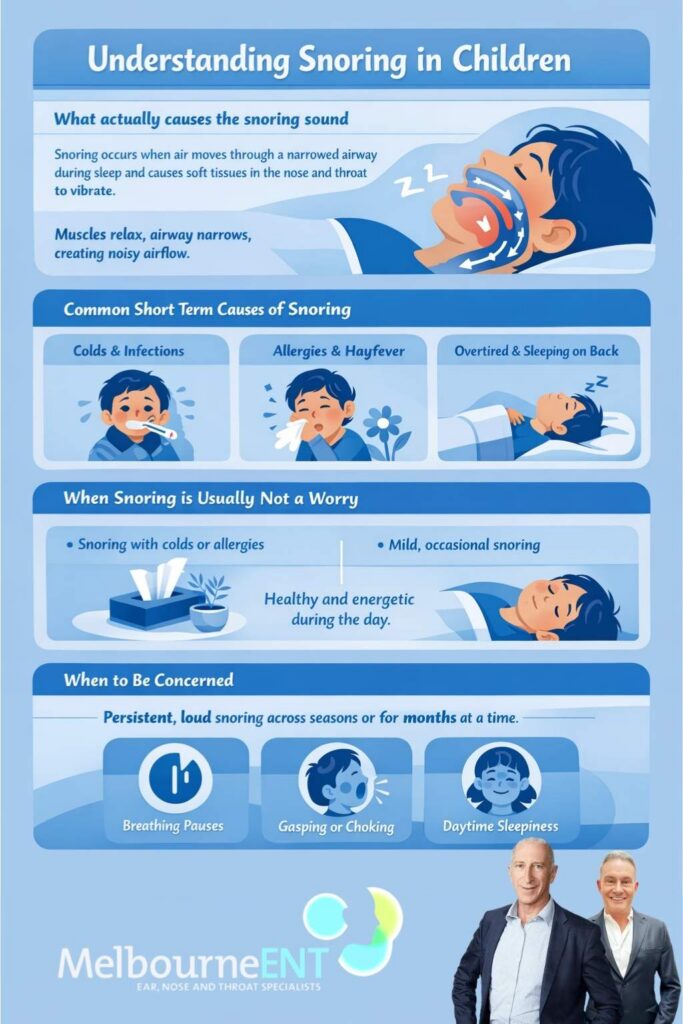
Snoring occurs when air moves through a narrowed airway during sleep and causes soft tissues in the nose and throat to vibrate. In children, this airway includes the nose, the back of the mouth, the tonsils, the adenoids and the upper part of the windpipe.
When a child is awake and the muscles are active, the airway tends to stay open. When they fall asleep, the muscles relax. If the airway is already a bit crowded, for example by enlarged tonsils or adenoids or by swollen nasal lining, that relaxation can cause the space to become even tighter. As air is drawn through this narrow passage, it becomes turbulent and creates the snoring sound.
Occasional snoring when a child has a cold or is extra tired can be normal. Regular loud snoring on most nights is more likely to signal that the airway is consistently restricted.
✓ Common short term causes of snoring
Short term snoring is often due to conditions that resolve on their own. Viral infections that cause blocked noses, sore throats and fevers frequently lead to a week or two of noisy breathing. As the infection settles and swelling in the nose and throat reduces, snoring usually disappears.
Hayfever is another common contributor. In Melbourne, many children experience seasonal allergic rhinitis in spring and summer. Swelling and congestion in the nasal passages can force a child to breathe through the mouth, especially at night. This mouth breathing can be noisy and can dry the throat, making snoring more obvious while the allergy is active.
Sleeping flat on the back, having a very long or busy day or being overtired can also make snoring temporarily worse by relaxing the airway muscles more deeply.
✓ When snoring is usually not a worry
If snoring appears only during colds or intense allergy flare ups, and if your child is otherwise healthy and energetic during the day, it is often reassuring. Many parents will notice a noisy week or two each winter or hayfever season and then find that their child returns to quiet sleep.
Mild, infrequent snoring without any pauses in breathing, gasping or choking, and without daytime behaviour or learning issues, is usually not a cause for alarm. In these cases, your GP may suggest simple measures such as treating allergies, using saline sprays, adjusting sleep position and then watching how things evolve over time.
Persistent, loud snoring that continues across seasons or for months at a time is different. That is when it becomes important to think beyond short term causes.
When Summer Snoring Might Be More Than Allergies
✓ Why parents often “blame” allergies
In a city where hayfever is so common, it is natural to link summer snoring with allergies. If your child has itchy eyes, a runny nose and sneezing, and they snore more when pollen counts are high, allergies are almost certainly involved. Many parents and even some children see this pattern as normal and something to be endured each year.
Because allergies are so familiar, it is easy to overlook other contributors. If snoring has been present at a low level throughout the year, the extra noise in summer may simply draw attention to a problem that has been there for longer.
✓ Clues that it may not be just hayfever
Certain features suggest that snoring might be more than seasonal hayfever. If your child snores loudly most nights of the week, even when other allergy symptoms are mild, that is one clue. If you can hear the snoring from another room with the door closed, or if siblings complain about the noise, it may be more than a blocked nose.
Another clue is persistence beyond the pollen season. If your child continues to snore heavily in late autumn or winter when hayfever usually settles, it becomes less likely that allergies are the only cause. Snoring that does not improve despite appropriate allergy medications from your GP or paediatrician also points to other factors.
✓ The overlap: allergies plus structural blockage
Allergies and structural narrowing often overlap. A child may have swollen nasal tissue from allergic rhinitis and also have enlarged adenoids blocking the back of the nose. They may have a history of hayfever alongside large tonsils that crowd the throat. In these situations, treating allergies can help but may not fully resolve the problem because there is still not enough room for air to flow freely.
Recognising this overlap is the key to bridging from the idea of simple allergy related snoring into a broader view that includes tonsils, adenoids and sleep disordered breathing.
Bridging Into Tonsils, Adenoids, Sleep Disordered Breathing And ENT Assessment
✓ What are tonsils and adenoids
Tonsils are small masses of lymphoid tissue located at the back of the throat, one on each side. They sit just behind the tongue and can usually be seen when a child opens their mouth wide. Adenoids are made of similar tissue but are located higher up, behind the nose where the nasal passages meet the throat. They cannot be seen directly during a routine examination without special instruments.
Both tonsils and adenoids are part of the immune system and are usually largest in early childhood, when the immune system is learning to recognise many new germs. As children grow older, these structures often shrink relative to the size of the surrounding airway.
✓ How enlarged tonsils and adenoids affect breathing
In some children, the tonsils or adenoids, or both, become significantly enlarged. This may be due to repeated infections, ongoing immune stimulation or a tendency for lymphoid tissue to overgrow. When enlarged, tonsils protrude into the space where air passes from the mouth into the throat, and adenoids extend into the back of the nasal cavity.
While the child is awake and upright, air may still pass through these narrowed channels without too much difficulty. When they lie down and fall asleep, the muscles of the throat relax and the tongue moves slightly backwards. The combination of relaxed muscles and bulky tissue can reduce the space dramatically. Airflow becomes noisy. In more severe cases, the airway may briefly collapse, causing pauses in breathing that are followed by a gasp or snort.
✓ What is sleep disordered breathing
Sleep disordered breathing describes a range of problems with breathing during sleep. At the milder end is simple snoring, where airflow is noisy but not seriously disrupted. As the problem becomes more severe, children may develop obstructive sleep apnoea, where the airway repeatedly narrows or closes and breathing stops for several seconds at a time.
Children with sleep disordered breathing often have fragmented sleep, even if they appear to sleep through the night. They may move a lot, sweat, wake briefly without remembering it or assume unusual positions to help keep their airway open. These repeated disturbances can affect the quality of sleep and lead to daytime symptoms.
It is not possible for parents to diagnose obstructive sleep apnoea reliably at home, but they can notice patterns and share them with their GP. From there, an ENT specialist can investigate further.
✓ Why an ENT specialist is well placed to assess this
ENT surgeons specialise in conditions of the ear, nose, throat and related structures. They are trained to assess the airway comprehensively and to identify anatomical and functional problems that may contribute to snoring and sleep disordered breathing.
At Melbourne ENT, Dr Stephen Kleid and Dr Simon Braham regularly review children with snoring and suspected sleep disordered breathing. They assess the size and position of the tonsils, look for signs of enlarged adenoids, examine the nasal passages and consider jaw and palate shape. They also take into account allergy history, recurrent infections and any other relevant medical issues.
This detailed assessment allows them to recommend a management plan that may include medical treatment, watchful waiting or surgery, depending on the severity of the problem and the needs of the child.
Signs Parents Can Watch For At Home
✓ Night time signs of possible sleep disordered breathing
At home, you are the person who sees your child as they actually sleep. Signs that deserve attention include loud snoring on most nights, especially if it has been present for several months. Pauses in breathing, followed by a gasp, snort or sudden movement, are particularly important.
Other possible signs are restless sleep, frequent position changes and night sweats. Some children may sit up or hang their head over the side of the bed in an effort to breathe more easily. Persistent mouth breathing with the neck extended can also be a clue that the airway is narrowing during sleep.
✓ Day time signs that may be related to poor sleep
During the day, children with disturbed sleep can present in very different ways. Some are obviously tired, difficult to wake in the morning and sluggish during the day. Others seem overactive, impulsive or emotional. Teachers may report problems with concentration, memory or behaviour, sometimes without realising that sleep might be part of the underlying cause.
Morning headaches, a persistently dry mouth or ongoing mouth breathing are other signs that may accompany poor quality sleep. Over time, untreated sleep disordered breathing can affect growth, learning and general wellbeing.
✓ When urgent medical care is required
Most snoring does not require emergency treatment. However, if your child is having obvious trouble breathing, is making very little air movement, has blue or grey lips, or is extremely difficult to wake, you should seek urgent medical help and call emergency services or attend the nearest emergency department.
This article offers general information only. It does not replace a medical assessment. If you are worried about your child’s breathing for any reason, it is always better to seek medical advice.
The Role Of Your GP In First Line Assessment
✓ Starting the conversation with your family doctor
Your GP is usually the first person to speak to if you are worried about your child’s snoring. Bringing a simple sleep diary or short video clips recorded on a phone can be very helpful. These can show how loud the snoring is, how often it occurs and whether there are pauses in breathing.
The GP will ask about allergy symptoms, past infections, growth, weight and general health. They will examine your child’s nose, throat and ears and listen to their chest. This helps to identify whether the problem is likely to be due to allergies, infection, asthma or a more structural issue in the airway.
✓ When a GP might suspect something more
If snoring is persistent and loud, if there are any reports of breathing pauses, or if teachers or carers have expressed concerns about behaviour or learning, your GP may suspect sleep disordered breathing. Recurrent tonsillitis, frequent ear infections or long standing nasal blockage can also raise suspicion of enlarged tonsils or adenoids.
In these situations, the GP may start by optimising medical treatment, for example by improving allergy control. If, despite this, snoring and sleep problems continue, they may recommend referral to an ENT specialist at a clinic such as Melbourne ENT in St Kilda East.
✓ Referral and Medicare rebates
In Australia, a referral from a GP or another specialist is usually needed to see an ENT surgeon and to claim Medicare rebates for consultations. The referral outlines your child’s medical background and the main reasons for seeking specialist input.
Medicare provides a rebate for part of the cost of seeing an ENT specialist. The exact out of pocket cost will depend on the practice fees and any private health insurance you may have. The staff at Melbourne ENT can explain how referrals and rebates work for their clinic and help you understand the likely costs for consultations and any recommended procedures.
What Happens At An ENT Assessment At Melbourne ENT
✓ The initial appointment
At Melbourne ENT, the first consultation is focused on gaining a clear picture of your child’s symptoms and general health. The surgeon will ask when the snoring started, how often it occurs, how loud it is and whether you have noticed pauses in breathing or unusual sleep behaviours. They will also ask about daytime tiredness, behaviour, school performance, recurrent sore throats, ear infections and nasal congestion.
The clinic environment in St Kilda East is designed to be calm and child friendly. Children are encouraged to ask questions and to be involved in a way that suits their age. Parents can share concerns openly so that the surgeon understands not just the physical symptoms, but also the impact on family life.
✓ ENT examination
The physical examination involves looking into the ears with a light, examining the nose and throat and feeling the neck for enlarged glands or other lumps. The surgeon will assess how large the tonsils are and how much they narrow the airway. They will look for signs of chronic infection or inflammation.
The nasal passages are examined for swelling of the lining, nasal polyps or deviation of the septum. In some children, a small flexible camera may be used to look at the adenoids and the back of the nose. This is usually a quick procedure and is explained carefully to help your child feel as comfortable as possible.
✓ Additional investigations when needed
Not every child who snores needs further tests, but in certain circumstances an overnight sleep study or other monitoring may be recommended. This is more likely if symptoms are severe, if there are other medical conditions present, or if it is difficult to judge how significant the breathing disturbances are from examination alone.
Sleep studies are usually organised in collaboration with paediatricians and sleep specialists. They provide detailed information about breathing, oxygen levels and sleep stages throughout the night and can help guide treatment decisions.
✓ The experience and expertise of the surgeons
Dr Stephen Kleid’s long standing work as an ENT and Head & Neck Surgeon, including roles at Royal Melbourne Hospital and Peter MacCallum Cancer Centre, has given him broad experience in both complex and common conditions of the head and neck. This depth of expertise helps in assessing each child thoroughly and in discussing the safest and most appropriate options.
Dr Simon Braham has many years of experience in ENT practice across Melbourne and regional Victoria. His ongoing work in hospitals such as the Royal Victorian Eye and Ear Hospital has included a strong focus on nasal, sinus and paediatric ear, nose and throat surgery.
At Melbourne ENT, both surgeons aim to explain findings clearly, listen to family priorities and provide realistic advice about what to expect from various treatments.
Treatment Options: From Medical Management To Surgery
✓ Addressing allergies and nasal obstruction
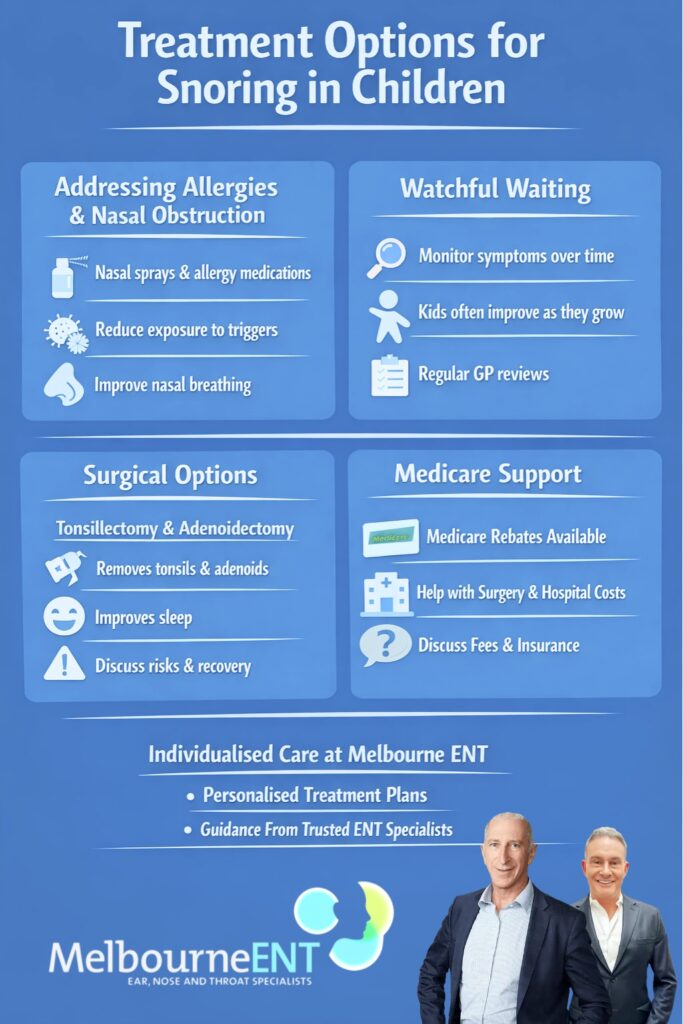
For many children, the first step in managing snoring and sleep disordered breathing is to improve nasal airflow and control allergies. This can involve regular use of saline sprays or rinses, intranasal corticosteroids prescribed by a doctor, and other allergy medications where appropriate. Reducing exposure to known triggers, such as dust mites or pollen, may also help.
Improving nasal breathing can reduce mouth breathing and snoring for some children. It also allows the ENT specialist to see how much of the problem remains once allergies are under control. If snoring continues at a significant level despite good medical treatment, then enlarged tonsils or adenoids may still need to be addressed.
✓ Watchful waiting and monitoring
If a child’s symptoms are mild, and if examination suggests only moderate enlargement of tonsils or adenoids, it may be reasonable to adopt a watchful waiting approach. Children grow, their faces and jaws develop and their airways often become relatively larger with time. Tonsils and adenoids can also shrink relative to the airway as a child gets older.
During a period of observation, your GP and the team at Melbourne ENT may suggest regular reviews to monitor snoring, behaviour and general health. Parents play a key role by reporting any change in symptoms. This approach avoids unnecessary surgery while ensuring that any deterioration is picked up early.
✓ Surgical options: tonsils and adenoids
When enlarged tonsils and adenoids clearly contribute to significant sleep disordered breathing or recurrent infections, surgery may be recommended. An adenoidectomy is the removal of the adenoids from the back of the nose. A tonsillectomy removes the tonsils from the back of the throat. An adenotonsillectomy removes both the tonsils and adenoids in one procedure.
The intention of these operations is to open up the airway and allow smoother airflow during sleep. Many children who undergo these surgeries sleep more quietly, wake more refreshed and show improvements in mood and concentration. However, results vary, and some children may still snore occasionally, especially during colds or allergy flares.
All operations involve potential risks. After tonsil and adenoid surgery, common issues include throat pain, temporary difficulty swallowing and a period off school. There is also a risk of bleeding during or after the operation, infection and very rarely more serious complications. These risks are always discussed with parents so that they can weigh them against the expected benefits.
Medicare plays an important role in helping families manage the costs of these procedures in Australia. Tonsillectomy, adenoidectomy and adenotonsillectomy are listed under the Medicare Benefits Schedule when they are medically indicated and performed by a specialist. Medicare provides a rebate for part of the surgeon’s fee and contributes to anaesthetist and hospital costs. The final out of pocket amount will depend on the surgeon’s fees, the hospital used and whether you have private health insurance and what that insurance covers. The team at Melbourne ENT can give you general information about typical fee structures and guide you to confirm specific rebate and gap details with Medicare and your health fund before making decisions about surgery.
✓ Individualised decision making at Melbourne ENT
Every child is different. At Melbourne ENT, Dr Stephen Kleid and Dr Simon Braham consider each child’s overall health, severity of symptoms, examination findings and test results before recommending any treatment path.
Parents are central to this process. The surgeons will explain all available options, including ongoing medical therapy, observation and surgery if indicated. They will discuss what each option might mean for your child’s sleep, school attendance and recovery and which hospital is likely to be most appropriate, such as Masada Private Hospital or another accredited facility in Melbourne.
This collaborative approach helps ensure that families feel informed and supported at every step.
Recovery, Follow Up And Long Term Outlook
✓ After medical treatment or surgery
If your child has surgery, the recovery period is a vital part of the process. After an adenotonsillectomy or related procedure, your child will usually need pain relief, plenty of fluids and time at home to rest. Eating may be uncomfortable for a while, and it is normal for children to be more tired and clingy during this period.
The Melbourne ENT team will provide written and verbal instructions about caring for your child at home and what warning signs to watch for, especially signs of bleeding or dehydration. Follow up appointments are used to check healing and to discuss how sleep and daytime functioning are changing.
For children managed with medical treatment alone, follow up focuses on symptom control and monitoring for improvement or deterioration. Treatment plans may need adjustment over time, especially as children grow and seasons change.
✓ Monitoring sleep and daytime functioning
After treatment, it is helpful to keep paying attention to your child’s sleep and daytime behaviour. Parents often notice changes gradually, such as quieter nights, easier mornings, better mood and more consistent school performance. Teachers may also report improvements.
If you notice that snoring remains loud and frequent, that breathing pauses continue, or that daytime problems persist, it is important to raise this with your GP or the team at Melbourne ENT. Some children, particularly those with additional medical issues or weight concerns, may need further evaluation or ongoing support.
✓ Long term goals
The long term aim of assessing and treating snoring and sleep disordered breathing is to give children the best chance at healthy sleep, growth and development. Comfortable, regular breathing at night supports learning, emotional balance and general health.
It is also important to remember that no child sleeps perfectly every night. Occasional snoring during a cold or a particularly exhausting week is normal. The focus is on persistent patterns and their impact, not on eliminating every noise. With appropriate assessment and follow up, most children can achieve significant and lasting improvements.
Key Takeaways And Next Steps For Parents In Melbourne
✓ Key messages
Summer snoring in children is common, but when it is loud, regular and ongoing, it may be more than just allergies. Enlarged tonsils and adenoids, often combined with allergies and nasal obstruction, can cause sleep disordered breathing that affects a child’s mood, behaviour and learning.
Paying attention to patterns across seasons, not just isolated weeks, can help you decide when to seek help. Early assessment allows problems to be addressed before they cause long term difficulties.
✓ What to do if you are concerned about your child’s snoring
If you are worried about your child’s snoring, consider recording short videos of their sleep and keeping notes about how often snoring occurs and whether there are any breathing pauses. Take this information to your GP and discuss your concerns.
Your GP can assess for allergies, infections and other conditions and decide whether referral to an ENT specialist is appropriate. Remember that information online, including this article, is general. Decisions about your child’s care should always be made with your own doctors.

FAQs About Children’s Snoring In Summer And When It Is Not Just Allergies
Could my child still have a breathing problem at night if they fall asleep quickly and stay asleep all night?
Yes, it is possible. Some children with sleep disordered breathing fall asleep very quickly because they are overtired, and they may appear to sleep through the night without obvious awakenings. The concern is not just how many hours they are in bed, but how restful those hours are. Brief pauses in breathing and frequent mini arousals may not be obvious to parents, but they can still affect mood, attention and learning. If your child snores most nights, especially outside obvious allergy flare ups, it is sensible to discuss it with your GP even if they seem to sleep for a long time.
My child only snores when they sleep on their back in summer – is that enough to worry about?
Position related snoring is common, and for some children it is most noticeable when they lie flat on their back. If the snoring is mild, clearly linked to allergy days and not associated with breathing pauses or daytime problems, your GP may suggest simple steps such as improving allergy control and encouraging side sleeping. However, if back sleeping almost always triggers loud snoring, or if you notice pauses in breathing in that position, it can still be helpful to have an ENT assessment to check whether enlarged tonsils or adenoids are contributing to airway narrowing.
Can long term mouth breathing change the way my child’s face or teeth develop?
Long term mouth breathing in childhood can be associated with changes in facial growth and dental development. Children who constantly breathe through their mouth may develop a longer face, a narrow upper jaw or crowded teeth, although this does not occur in every case. If snoring, mouth breathing and nasal blockage are present for many months or years, it is reasonable to speak with your GP about an ENT review. In some situations, ENT specialists and dentists or orthodontists work together so that both airway health and dental alignment are considered.
Is it possible that my child’s behaviour or school difficulties are linked to snoring, even if no one has mentioned sleep problems before?
Yes, this can happen. Some children with sleep disordered breathing do not complain of feeling tired and do not fall asleep in the daytime, but they may show irritability, emotional ups and downs, difficulty concentrating or hyperactive behaviour. Teachers may focus on attention or behaviour without realising that sleep could be part of the picture. If your child snores regularly and you have concerns about their learning or behaviour, it is worth mentioning sleep when you speak with your GP, teacher or psychologist so that the possibility of disturbed sleep is not overlooked.
If my child has enlarged tonsils and adenoids, will they definitely need surgery at some point?
Not every child with large tonsils or adenoids needs surgery. Many children have moderate enlargement that does not cause significant symptoms and may improve with time as they grow. The decision to operate is based on the severity of snoring or sleep disordered breathing, the presence of recurrent infections and the overall impact on your child’s quality of life. At Melbourne ENT, surgeons such as Dr Stephen Kleid and Dr Simon Braham look at the whole picture, and may recommend ongoing monitoring rather than surgery if problems are mild.
Can allergies and enlarged tonsils or adenoids be treated at the same time, or do they need to be dealt with separately?
They can often be managed together. Treating allergies with appropriate medications and environmental strategies can improve nasal breathing and reduce some of the strain on the airway. Once allergies are well controlled, it is easier to see how much of the remaining problem is due to enlarged tonsils or adenoids. An ENT specialist can help you understand how much each factor contributes and can coordinate a plan with your GP or paediatrician so that allergies and structural airway issues are addressed in a logical and efficient way.
What if my child had their tonsils and adenoids removed but I still hear snoring during summer allergy flares?
Some children continue to snore occasionally after tonsil and adenoid surgery, especially when they have a cold or active allergies. In this situation the snoring may be mainly due to swelling of the nasal lining rather than continued obstruction from tonsils or adenoids. If your child is otherwise sleeping peacefully, waking refreshed and doing well at school, occasional snoring linked to illness or allergy is often not concerning. If loud snoring, breathing pauses or daytime difficulties return, it is important to let your GP or ENT specialist know so that your child can be reassessed and further options can be discussed if needed.
Medical References
- Snoring and Obstructive Sleep Apnea in Children / JAMA Otolaryngology / https://jamanetwork.com/journals/jamaotolaryngology/fullarticle/404567
- Approach to the Snoring Child / PubMed Central / https://pmc.ncbi.nlm.nih.gov/articles/PMC7905134/
- Childhood Snoring Cannot Be Ignored / Sleep Journal / https://academic.oup.com/sleep/article/45/5/zsac045/6535538
- Incidence and Prevalence of Snoring In Paediatric Patients / Journal of Clinical Case Reports / https://jccpractice.com/article/incidence-and-prevalence-of-snoring-in-paediatric-patients-an-original-research-563/
- Behavioral Patterns in Children with Snoring / PubMed Central / https://pmc.ncbi.nlm.nih.gov/articles/PMC12731426/
- Prevalence of Snoring and Associated Factors / SAGE Journals / https://journals.sagepub.com/doi/10.1177/30502225251364962
- Loudness of Snoring in Pediatrics / Sleep Medicine / https://www.sciencedirect.com/science/article/pii/S1389945725000061
How Melbourne ENT can support your child
Melbourne ENT in St Kilda East provides comprehensive care for children with snoring, enlarged tonsils and adenoids and suspected sleep disordered breathing. With the experience of Dr Stephen Kleid, ENT and Head & Neck Surgeon, and Dr Simon Braham, ENT Surgeon, the clinic offers detailed assessment and a full range of treatment options, from medical therapies to surgery when suitable.
The surgeons at Melbourne ENT work closely with GPs, paediatricians and hospitals across Melbourne and Victoria to coordinate care. If you are concerned about your child’s snoring, you can speak with your GP about a referral to Melbourne ENT and visit related pages on the website for more information about services, surgery guides and what to expect from an ENT consultation.
Further Reading
- Read more about Adenoidectomy Melbourne
- Read more about Snoring – Sleep Apnoea
- Read more about Sleep Disturbed Breathing In Kids Melbourne
- Read Melbourne ENT’s Blog on Snoring Treatments – Causes, Risks and Options
Breathing Problems for Kids – Causes and Solutions
Breathing problems in children refer to any condition that makes it difficult for them to…
Using the STOP-BANG Questionnaire to assess Sleep Apnoea & OSA
Do You Have Sleep Apnoea or OSA? Find Out with the STOP-BANG Questionnaire If you…
Snoring Treatments – Causes, Risks and Options
Snoring is a real problem that can affect your sleep, your health, and your relationships….